Umbilical Hernia Repair
What does surgery involve?
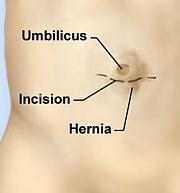
- Open Repair. This is preferred technique in most patients. The operation is done under a general anaesthetic. A small incision is around the umbilicus and the hernia is returned into the abdomen. The hole in the abdominal wall is closed with either Nylon sutures( if the defect is less than 2 cm) or with a patch of mesh made from a special plastic and the wound is closed with dissolving sutures. Steristrips (paper tape) and a water proof dressing is applied. Occasionally for large hernias that have been present for long time, this skin of the umbilicus can be very thin. When this happens it is better to remove the umbilicus all together to prevent that thinned out skin from dying and causing wound infection. I will warn you about this prior to surgery.
- Laparoscopic repair. This is used less frequently than in groin hernias. It is reserved for patients with large or recurrent umbilical hernias.
What are the complications of umbilical hernia repair?
Specific Complications:
- Bleeding: It is quite common to get some bruising near the wound. This is expected. However, more significant bleeding into the wound can occur and this may require a return to the operating theatre.
- Seroma formation: this is a temporary fluid collection at the site of the hernia. It is fairly common and tend to settle with time. However occasionally it need to be aspirated with a needle.
- Recurrence of the hernia: less than 10%.
- Mesh infection: This is very rare but may necessitate removal of the mesh by another surgery.
- Damage to bowel or other structures within the abdomen: This is a rare but serious complication. It requires repair with a bigger operation.
- Removing the umbilicus: If it looks like the skin will not survive after surgery
- Damage to bowel or urinary bladder: This is a rare complication can be serious and require repair with a bigger operation.
General Complications:
- Cardiovascular problems: heart attacks and strokes. Both are very rare.
- Respiratory problems: pneumonia and aspiration.
- Wound infection or urinary infection
- Clots in the legs that may travel to the lungs. This is a rare but serious complication.
- Wound pain and abnormal (keloid) scarring.
- Death from general anaesthetic. This is very rare (1 in 40,000).
- Chipped teeth and sore throat form the insertion of the breathing tube.
- Drug reactions.
Preparation for Surgery:
- Shower at home the morning of the operation
- Do not shave the surgery site! This will be done in the operating room. Shaving at home increase the chance of wound infection.
- You need to fast for 6 hours prior to surgery. The time to fast depend on the time of your operation and the hospital will notify about that time. Generally, for morning operations, you should fast from midnight the night before and for afternoon operations, you should have a breakfast at 6 AM then fast. You can still take your heart and blood pressure medications with a small sip of water.
- If you are diabetic let me and the anaesthetist know to advice you about changes to your medications.
- Do not smoke for 4 weeks before surgery. Smoking increases the complications.
- Do not drink alcohol for 24 hours prior to surgery.
- Let me and the anaesthetist know If you are on drugs that thin the blood. Some of these drugs need to be stopped or changed a week before surgery to reduce the risk of bleeding.
- Stop herbal medications for two weeks prior surgery. Medications like Garlic, fish oil, St John's Wort, Ginseng, Ginko can increase the risk of bleeding.
What to expect after surgery?
Most patients will be able to go home on the same day. Some patients will be kept in overnight.
Pain control: Local anaesthetic will be used in the wound. This will last for 6-12 hours. Panadol taken regularly is often enough to control the pain especially for key-hole surgery. If this is not enough then NSAIDs class drugs like Nurofen, Mobic, Brufen or Indocid can be used. These need to be used with caution in the elderly, patients with kidney disease and patients with peptic (stomach) ulcer disease.
Passing Urine: All patients must be able to pass urine after surgery prior to be sent home. If you have difficulty passing urine then having a warm shower often helps. Rarely a urinary catheter need to be inserted.
Wound Care: The stitches are internal and these will dissolve. There will be thin paper tapes (Steristrips) covering the wound and on top of that there will be a water proof dressing. It is ok to have a shower but pat the wounds dry with a towel afterward. Bruising at the site of the wound and the scrotum is expected and is normal as is some blood stained staining of the dressings. However, more significant bleeding requires medical attention and review. Remove the water proof dressing after five days. Leave the paper tapes until they fall by themselves. This will give you a better scar. Some thickening like a ridge under the wound is expected. This will soften with time. It is normal to have a patch of numbness under the wound. This will improve with time as well.
Activity: You should not drive for at least a week after surgery and when you can respond in an emergency. Walking and light activities are encouraged from day one. Light exercise can be resumed when you feel comfortable. This varies between patients and you should listen to your body. Heavy lifting (more than 10 kg) should be avoided for 6 weeks after open surgery and 2 weeks after laparoscopic surgery. Swimming can be resumed two weeks after surgery. Sexual activity can be resumes after one week.
When to return to work?
This depends on the job, level of activities and method of surgery (open versus laparoscopic). Desk jobs (light activities) can be resumes within one week. Jobs with moderate activities (lifting less than 20 kg) can be resumes with two weeks (one week for key-hole surgery). Heavy jobs with frequent lifting of more than 20 kg) can be resumes after three to four weeks (two weeks for key-hole surgery).
Follow-up:
I see most patients within 4-6 weeks after surgery. Usually one review is all that is needed and after that I see my patients on as needed basis. You should come and see me at any time if you one of the following:
- Fever >38 degrees or chills
- Increasing pain or redness around the incision
- Foul smelling or creamy wound discharge
- Increasing pain, nausea or vomiting
- If you are concerned about anything
