Within two to three days after your operation – depending, of course, on your condition and the assessment of Dr. Zarrouk – you will be allowed to return home, where you will continue with your liquid diet for some time. At first, this may consist of continuing to drink "free fluids," such as water, clear soups, milk, custard, diet cordials, or tea and coffee, as you were doing in the hospital. Again, don't feel in any need to rush things. Your aim should be to drink around two litres of fluid. Remember, your stomach capacity is very small now and your stomach is swollen and will not stretch. Therefore, you need to sip fluid all the time.
Experiment with liquids at different temperatures to see whether this makes a difference in your enjoyment of them; some people do better with warm liquids, while others prefer colder ones. You may also supplement the liquids with others approved by your doctor, such as unsweetened but flavoured mineral waters, diet (non-sugar) drinks, sugar-free gelatines, fat-free or low-fat clear (or strained) broths and soups, sugar-free Jelly, and sugar-free ice pops.
If you find that you tolerate them well, you can also try adding no-sugar-added (and pulp-free) vegetable juices, sugar-free fruit juices, or thin smoothies made by blending apples, strawberries, cranberries, bananas, or grapes, and then straining them before drinking them. Avoid strong, acidic fruit juices such as orange, grapefruit, or pineapple. You should not drink any fizzy (carbonated) drinks.
Moving to more varied liquids
As you become more accustomed to this diet, you may vary the fluids by adding protein shakes (e.g Optifast), milk, or other more substantial liquids to your diet. When choosing these protein drinks, make sure that they provide 20-30 grams of protein but less than 10 grams of sugar and less than 5 grams of fat. Again, start slowly and take your time. Your goal at first should be to drink at least 30 ml every 15 minutes, without gulping or trying to rush things.
Within a couple of days, however, you may start consuming these fluids on a more regular basis, as if they were your regular meals; i.e., three times a day, just as you would normally. It is important during this at-home period to begin to move towards a more normal eating schedule so that your new stomach becomes accustomed to it. Your other goal during this period – without forcing it – should be to consume approximately 2 litres of liquid per day.
During this phase of your recovery diet, it is normal to every so often take an overly-large sip of liquid and feel some momentary nausea. Having a stomach several times smaller than it was before takes some getting used to. If this happens, the best approach is to remain seated or standing upright rather than lying down, thereby allowing gravity to help pass the liquid through your stomach and into the lower intestinal tract.
No solid foods
You should not eat any solid food during this phase of your recovery period, no matter how much you may be tempted to do so. You should also not consume carbonated beverages, sugar-sweetened beverages, or alcohol. You should also avoid any high-fat or high-sodium broths, any soups that contain noodles or other "chunks" that have not been blended to liquefy them, and semi-solid foods such as yoghurt, ice cream, or puddings. You should not take antiinflamatory medications such as Voltren, Nurofen, Mobic ..etc. If you need to snack during this period, stick to sugar-free Jell-O or sugar-free ice pops.
Your Regular Medications
It is OK to take your regular tablets orally. Large tablets may need to be crushed however, slow release tablets should not be crushed. Use liguid formulation (e.g. Panadol Syrup) when available.
Most importantly, don't despair…you're more than halfway through the process and well on your way back to normal eating. In the next phase of your recovery, you'll be moving to the next phase of your limited diet and soon after that to an almost-normal diet.
By the end of the sixth week following your sleeve gastrectomy operation, you should be able to eat foods of a more normal consistency, without worrying about the "soft foods" restriction. However, as with previous phases of your recovery diet, it is important not to rush this step; you should only progress to this stage of your diet plan if you tolerated soft food well.
Remember the lessons learned
It is important during this phase to remember the lessons you have learned previously:
- Eat three meals a day on a regular basis. Do not skip breakfast or other meals. Each meal should be nutritionally balanced and contain sufficient protein.
- Choose small portions, and take tiny bites, chewing each bite thoroughly before swallowing it. Stop eating when you are full.
- Focus on healthy, balanced meals. This is the phase of your diet in which you are establishing the eating habits that you will follow for the rest of your life and that will enable you to end your obesity.
- Continue to drink lots of liquids. In general, it is still a good idea to not drink with meals; however, during the day, try to consume at least 1-1.5 litres of approved beverages.
- Nutritional supplements. Keep taking the daily vitamin supplements as before e.g. Centrum or Nutrichew.
- Avoid between-meal snacking. Small snacks as detailed below are OK, but eating constantly during the day is one of the habits you want to get over, not perpetuate.
- Get enough exercise. Balance your new healthier eating habits with healthy exercise.
Leave your old habits
Your Sleeve Gastrectomy surgery is permanent, so leave your old, unhealthy eating habits behind
The first year following Sleeve Gastronomy surgery is critical. The operation is permanent, but its success in achieving long-term weight loss goals can be sabotaged by holding on to old lifestyle habits such as constant snacking or "grazing," poorly balanced meals, lack of exercise, and poor food choices such as fast foods, alcohol, and sweets. This is your opportunity to start over and establish new healthy eating habits. You have the opportunity in this phase of your post-surgery diet plan to redesign your whole approach to eating. Foods that are ideal for this phase of your diet include:
- Protein – (2 servings a day) lean meats, chicken, fish, eggs, or legumes to keep your protein intake high so that weight loss does not cause muscle loss.
- Fruits and Vegetables – (2 servings a day) almost any vegetables, prepared steamed, boiled, broiled, or stir-fried with minimal added oils or butter.
- Milk and dairy products – (3 servings a day) skim or low-fat milk (max. 250 ml/day); cottage cheese, ricotta cheese, or low-fat cheese slices (max. 30 g/day) or low-fat yoghurt (max. 200 g/day).
- Breads and cereals – (3 servings a day) Look for high fibre and low sugar content, avoiding soft, doughy breads that expand in the stomach; low-fat crackers, multigrain breads, rice, pasta, noodles, Weetabix, or porridge.
- Fats – (maximum 2 teaspoons per day) olive oil, low-fat cooking spray, polyunsaturated or monounsaturated margarines; no butter or heavy oils.
Foods you should avoid
In this new "the rest of your life" diet, there are certain foods and drinks you should say goodbye to forever, either because they are bad matches for the size and sensitivity of your new, smaller stomach or because they are bad for your health and weight loss goals.
- Avoid alcoholic drinks and any sugar-sweetened teas, coffees, or soft drinks.
- Try to avoid fresh, doughy breads and carbohydrates (because they swell in the stomach).
- Avoid sugar and sweets such as ice cream, milkshakes, chocolate, flavoured milks, pastries, cakes, biscuits, and lollies.
- Try to avoid the use of oils in cooking, and avoid deep-fried foods.
- Stay away from fast food and commercial snack foods.
Instead, concentrate on developing protein-rich, balanced meals made from fresh foods whenever possible (as opposed to canned or pre-prepared). Remember when selecting and preparing these foods that your original goal in having the Sleeve Gastrectomy operation was to lose weight and end your obesity forever.
We recommend that you keep a journal of your dietary choices during this first year after surgery so that you can review it with Dr. Zarrouk and the dietitian and relate those choices to the speed of your weight loss. The sleeve gastrecotmy operation will help by limiting the amount of food you can eat and that you need to feel full and satisfied. However, your weight loss process can go faster by making wise, healthier choices in the types and amounts of foods you do eat.
This is literally your opportunity for a new start in life. Good luck, and do not hesitate to contact us at any time if we may be of assistance.
What to Bring to Hospital
- Any medications you take (in their original boxes/bottles).
- Scans you've had done with Dr. Zarrouk or Dr. Kirby.
- Comfortable clothes or pyjamas to walk around the ward.
- Comfortable shoes/slippers.
- Toiletries.
- Fiji water (many people find Fiji water easier to drink than regular water).
- Diet cordial or similar to mix into water, making it easier to drink.
- CPAP machine if you use one for sleep apnoea.
- Bring comfortable clothes and shoes for walking.
- Pack toiletries and any medications you take.
- Consider bringing Fiji water or diet cordial to make drinking easier.
Admission Through to Post-Op
- Day Before Surgery: The hospital will inform you of your arrival and fasting times.
- Arrival: Go to the front desk to be admitted through the Day Surgery Unit.
- Preparation:
- Change into a hospital gown.
- Put on TED stockings.
- Transfer to Surgery:
- A wardsman will take you on a bed to the anaesthetic bay.
- Wait until they are ready to begin surgery.
- Recovery:
- Spend at least 1 hour in the Recovery Ward post-surgery.
- You will be transferred to either the High Dependency Unit (HDU) or a monitored surgical bed.
- After Arrival at Surgical/HDU Ward:
- Nurses will notify your Next of Kin.
- You will be connected to a heart monitor, blood pressure monitor, and oxygen saturation monitor until the following day (can be disconnected for walking).
- Intravenous fluids will be provided to keep you hydrated.
Triflow Incentive Spirometer
- Purpose: Helps open small air spaces in the lungs and clear secretions, preventing chest infections.
- How to Use:
- Exhale completely.
- Place your lips around the mouthpiece.
- Inhale deeply, aiming to lift all three balls and hold for a few seconds.
- Use 5 times every hour while awake.
- Reminder: Take the device home and continue using it for at least 2 weeks.
- Use the device 5 times every hour while awake.
- Take it home and continue using it for 2 weeks.
Mobility
- Importance: Start mobilizing as soon as it is safe after surgery.
- Helps expand your lungs.
- Restores circulation to your legs and extremities.
- Alleviates gas pain.
- Start walking as soon as it is safe after surgery.
- Walking helps prevent complications like blood clots and lung infections.
Medications
- Paracetamol:
- Initially given through IV.
- From the day after surgery, given in liquid form to drink.
- Pain Relief:
- Gas pain may occur (usually in the chest or shoulder tips) due to carbon dioxide gas from surgery.
- Ask your nurse for Oxynorm Liquid if strong pain relief is needed.
- Anti-Nausea Medication:
- Given through IV.
- Ask your nurse if you still feel nauseous.
- Nexium (for reflux and staple line healing):
- Given through IV twice a day while in hospital.
- Switch to tablet form for 3 months after discharge.
- Blood Thinning Injections:
- Prevent blood clots.
- Administered during the hospital stay.
- Diabetic Patients:
- May be put on a sliding scale of insulin (even if not normally required).
- Blood sugar levels will be checked every 4-6 hours, and insulin will be given as needed.
- Take Nexium for 3 months to help with reflux and healing.
- Ask for Oxynorm Liquid if you experience severe gas pain.
Prevention of Blood Clots (DVT & PE)
- TED Stockings: Wear in the hospital and continue wearing for 2 weeks at home.
- Pneumatic Calf Compressors: Worn during the operation and remain on until the morning after surgery.
- Blood Thinners:
- Heparin or Clexane administered in hospital.
- Clexane injections to be continued at home once a day for 2 weeks.
- Wear TED stockings for 2 weeks after surgery.
- Continue Clexane injections at home for 2 weeks.
Diet
- After Surgery: Begin with clear fluids.
- Day After Surgery:
- Progress to free fluids.
- Take small sips only.
- Avoid straws to prevent gas buildup.
- Discharge Requirement:
- Drink at least 1L of water in 24 hours.
- Mix apple juice or diet cordial with water to make it easier to drink.
- Start with clear fluids and progress to free fluids.
- Take small sips and avoid straws.
- Mix apple juice or diet cordial with water to make drinking easier.
General Post-Operative Advice
- Start slowly with sipping water and other clear fluids.
- Be aware that your stomach is swollen and tender, so it may be difficult to consume large quantities at first.
- Tips for Drinking:
- Take small sips and stop if you feel nauseous or full.
- Avoid gulping or drinking a whole glass quickly.
- Sip other liquids like clear soups, jellies, milk, custard, diet cordials, tea, and coffee slowly.
- Suck on ice cubes if feeling dehydrated.
Discharge
- Instructions: Refer to the Bariatric Surgery Discharge and First 2 Weeks Instructions.
- Medications: The hospital will provide scripts for medications upon discharge.
- Appointments: You will be given your first follow-up appointments before leaving the hospital.
- Follow the discharge instructions carefully.
- Take all prescribed medications as directed.
- Attend your follow-up appointments as scheduled.
Key Reminders
- Sip, Sip, Sip: Stay hydrated by sipping fluids slowly.
- Walk, Walk, Walk: Mobilize as soon as it is safe.
- Breathe, Breathe, Breathe: Use your triflow device regularly.
- Stay hydrated by sipping fluids slowly.
- Walk regularly to aid recovery.
- Use the Triflow device to prevent chest infections.
Why Follow a Pre-Op Diet?
Before your weight loss surgery, we recommend a Very Low Calorie Diet (VLCD) such as Optifast for 1 to 3 weeks. This diet helps shrink the liver and reduce internal fat, making gastric sleeve or gastric bypass surgery safer and more technically straightforward.

Step 1: Watch the Dietitian Pre-Op Class
You must watch our pre-operative dietitian class before your surgery.
Click here to watch the Pre-Op Diet Class
What Is the Optifast VLCD?
Optifast is a medically formulated meal replacement program that provides controlled amounts of protein, minimal carbohydrates, essential fats, and complete vitamins and minerals.
Optifast helps switch the body from burning carbs to burning fat — especially the fat surrounding the liver. This makes surgery technically easier for your surgeon.
Allowed vs Not Allowed Foods
Allowed Foods
- Low-starch vegetables: alfalfa sprouts, asparagus, bean sprouts, bok choy, broccoli, brussels sprouts, cabbage, capsicum, carrots, cauliflower, celery, cucumber, eggplant, green beans, konjac noodles, lettuce, leeks, mushrooms, onions, radish, shallots, silver beet, snow peas, spinach, squash, tomatoes, watercress, zucchini
- Soups: stock cubes, Bonox (in moderation), vegetable soups made from allowed vegetables, miso soup
- Sauces & condiments: lemon & lime juice, vinegar, Worcestershire sauce, Tabasco sauce, soy sauce (in moderation), chilli, diet/fat-free salad dressings, mustard, tomato paste
- Herbs & spices: all spice, basil, celery flakes, chilli, chives, cinnamon, cloves, coriander, cumin, curry powder, dill, fennel, garlic, ginger, lite salt, mint, mustard seed, nutmeg, oregano, paprika, parsley, pepper, rosemary, sage, thyme, turmeric, tarragon
- Miscellaneous: artificial sweeteners, sugar-free lollies & gum, diet jelly, flavour essences, diet toppings
- Low-energy drinks: water, soda water, diet soft drinks & cordial, plain mineral water, tea & coffee (30 mL skim milk, no sugar), herbal teas
- Fruits in limited quantities: up to 5 strawberries, 1 passionfruit, or 1 lime per day
Not Allowed Foods
- Corn, green peas, legumes, lentils, potato, sweet potato, parsnip, pumpkin, turnip
- All soups not based on allowed vegetables
- Cream, high-calorie simmer sauces and salad dressings
- Fruit juice, alcohol, regular soft drinks, cordial (with sugar)
- Dairy products: milk, cheese, yoghurt, cream, ice cream
- Biscuits, cakes, crackers, lollies, desserts (unless sugar-free)
- All fruits not listed in the limited allowance
Daily Guidelines for the Optifast Diet
- ✅ 3 Optifast products (any combination of shakes, bars, soups, or desserts)
- ✅ 2 to 6 cups of low-starch vegetables
- ✅ 1 serve of lean protein (e.g. 80 g cooked meat or tofu)
- ✅ 1–2 teaspoons of olive oil
- ✅ 3 litres of total fluid intake (including water, tea, shakes, etc.)
Note: The water used to make shakes or soups does not count toward your daily 2 litres of extra water.
Common Side Effects and How to Manage Them
- Fatigue, hunger, headache → Stay well hydrated with at least 2 litres of water
- Constipation → Add Benefiber to shakes
- Bad breath (halitosis) → Sugar-free gum or mints can help
- Lactose intolerance → Use Lacteeze drops or try bars/soups that are better tolerated
- Gluten-free → Optifast shakes and bars are gluten-free
Important for Diabetic Patients
- Your blood sugar levels must be closely monitored
- Your diabetes medications may need adjusting to avoid hypoglycaemia
Sample Meal Plan
| Meal | Sample Plan 1 | Sample Plan 2 |
|---|---|---|
| Breakfast | Optifast shake with water, ice + instant coffee | Optifast shake |
| Morning Tea | ½ Optifast bar + tea/coffee (30 mL skim milk) | Tea/coffee + 5 strawberries |
| Lunch | 1 Optifast soup | Salad + tuna + oil & vinegar |
| Afternoon Tea | ½ Optifast bar + tea/coffee | 1 Optifast bar |
| Dinner | 2 cups stir-fry veg + 80 g lean meat + 1 tsp olive oil | 1 Optifast soup + salad |
| Supper | Herbal tea + 125 mL diet jelly | Herbal tea |
Daily Summary Checklist
- ✅ 3 Optifast products
- ✅ 2–6 cups of allowed vegetables
- ✅ 1 serve of lean protein
- ✅ 1–2 teaspoons olive oil
- ✅ 3 L of fluid (including the liquid in shakes)
- 💡 Add Benefiber or Metamucil to your shakes to help prevent constipation
Frequently Asked Questions
Can I drink coffee or tea? Yes – black or with 30 mL of skim milk. No sugar.
What if I miss a shake? Try not to skip. Missing meals may cause tiredness or hunger.
Can I flavour my shakes? Yes – use sugar-free essences, add instant coffee, or blend with ice.
If you do not tolerate Optifast or other diet shakes, we offer a food-based pre-operative diet plan as an alternative. Please contact our clinic to discuss this option with our team.
What if I feel unwell? Contact our clinic or your GP if you have any concerns.
Comparison of Bariatric Procedures
| Name of Operation | Gastric Banding | Sleeve Gastrectomy | Gastric Bypass |
|---|---|---|---|
| Image | 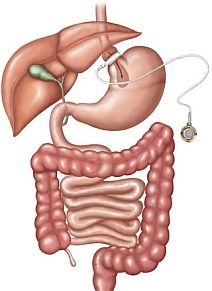 |
 |
 |
| How is it done? | Keyhole surgery | Keyhole surgery | Keyhole surgery |
| Modality of Weight Loss | Restrictive only | Restrictive and Metabolic | Restrictive and Metabolic |
| How does it work? | An inflatable band is placed around the top part of the stomach, limiting food intake by creating a sensation of fullness. The band is adjusted via an access port under the skin. Frequent adjustments are required. | The stomach is reduced to a narrow tube by removing 75% of the outer part. This limits food intake without obstruction and reduces ghrelin (a hunger hormone). | The stomach is reduced to a small pouch and connected to the small intestine. Food bypasses part of the digestive system, creating a strong hormonal response that suppresses appetite. |
| Operating Time | 1 hour | 2 hours | 2-3 hours |
| Advantages |
Removal possible (leaves a scar) No cutting or stapling needed Low early complication risk Easy procedure |
Reduces hunger Normal sensation of fullness No food intolerance No adjustments needed No foreign body Improves diabetes Less follow-up required "Set and forget" operation Easy to live with |
Reduces hunger Best long-term data Rapid initial weight loss Improves diabetes quickly Fixes acid reflux |
| Disadvantages & Complications |
Food intolerance Band erosion Slippage Hinders future surgeries Frequent reflux |
Staple line leak Narrowing Acid reflux (rare) |
Staple line leak Narrowing Ulcers Dumping syndrome Vitamin deficiencies Internal hernias Requires long-term follow-up |
| Vomiting | Very frequent | Very rare | Very rare |
| Long-term Need for Re-operation | 1 in 5 to 1 in 3 patients | Very rare | 5-10% over ten years |
| Average Hospital Stay | 1 Night | 2-3 Nights | 3-4 Nights |
| Quality of Life |
Poor Many struggle to eat healthy food |
Best among weight loss operations |
Good Dumping syndrome can be an issue |
| Average Weight Loss (Results may vary) |
30-40% of excess weight | 60-70% of excess weight | 60-80% of excess weight |
| My Recommendation | Avoid this operation! | Recommended for most patients | Consider if unable to have sleeve operation or for poorly controlled diabetes. |
Reference:
1. Diamantis T, Apostolou KG, Alexandrou A, Griniatsos J, Felekouras E, Tsigris C. Review of long-term weight loss results after laparoscopic sleeve gastrectomy. Surg Obes Relat Dis. 2014;10(1):177-183.